Contents>> Vol. 1, No. 2
Singapore’s Prescription for Successful Control of Transnational Emerging Infectious Diseases*
Minako Jen Yoshikawa**
**吉川みな子, Center for the Promotion of Interdisciplinary Education and Research, Inter-Graduate School Unit for Sustainable Development and Survival Societies, Kyoto University, 4 Ushinomiya-cho, Yoshida Sakyo-ku, Kyoto 606-8302, Japan
e-mail: mjenyjp[at]gmail.com
DOI: doi.org/10.20495/seas.1.2_301
Severe acute respiratory syndrome, a previously unknown emerging infectious disease, spread to multiple locations across continents in 2003 without being initially identified as a life-threatening infectious disease. The Republic of Singapore, in Southeast Asia, was one of the countries/areas affected by the global outbreak. With almost no existing procedures on how to deal with an emerging epidemic of such severity and rapid transmission, the country managed to formulate and implement policies to support countermeasures against this infectious disease. The interventions by the Singapore government covered of social and economic issues beyond the scope of public health, and promoted the involvement of governmental bodies and the general public. This example set by Singapore has been well recognized by international communities as the employment of successful containment measures. By scrutinizing public health measures deployed by the country, this paper identifies a political will that was embodied in a total governmental approach toward the emerging infectious disease in 2003; analyzes the origin of governmental intervention in health matters in the Republic; and shows why this country must choose to fiercely fight against health threats.
Keywords: Singapore, SARS, emerging infectious disease, Global City, transnational, political will, total governmental approach
I Introduction
In 2003, severe acute respiratory syndrome (SARS) emerged as a serious threat to worldwide health, resulting in 8,096 cases of infection and claiming 774 lives in 29 countries and areas.1) Singapore fell prey to SARS between March and May 2003, reporting 238 infected people and 33 deaths. Hidden from human eyes, the entirely unknown emerging infectious disease (EID) of “the age of globalization” imposed political, economic, and social threats in addition to medical challenges (World Health Organization (WHO) 2006, viii).2) The spread of SARS in urban, developed, and modern healthcare settings raised concerns globally. At the same time, the social attention to strict countermeasures imposed by governments also increased.3) The primary purpose of this paper is to analyze factors contributing to the success. I will, in particular, evaluate the influential role of the Singapore govern ment in implementing infectious disease intervention. The government gained recognition for its effective containment of the spread of SARS. The secondary purpose is to elucidate motives behind the proactive public health management in the Republic, which have existed since the inception of the young nation.
Before I proceed further, it is helpful to review two misconceptions pertaining to infectious diseases in developed economies such as modern Singapore. The first misconception is that infectious diseases no longer threaten the developed world, due likely to the perceived association between poverty and disease burden. In reality, developed nations are not free from serious threats of infectious diseases. In 1996, an enterohemorrhagic Escherichia coli O157 outbreak affected 9,451 patients and caused 12 deaths in Japan, then the second largest economy in the world. The O157 serotype caused morbidity numbering in the thousands in subsequent years in Japan (Machida 2005, 113–117).4) In 2007, media reports on methicillin-resistant Staphylococcus aureus infection caused fear in the United States.5) In 2009, the pandemic H1N1 influenza quickly spread beyond national and other territorial borders to affect both developed and developing areas globally.
The second misconception is that developed countries can easily control disease outbreaks. While superior healthcare facilities, laboratory capacities, and qualified professionals can contribute to effective responses vis-à-vis infectious diseases, engaging in active infectious disease management is largely at the discretion of individual governments. Governments might, therefore, choose to direct their full attention to other political agendas despite the new International Health Regulation 2005 requiring each member state to fulfill its responsibility. Additionally, high-quality healthcare is not synonymous with an ability to easily overcome infectious diseases. This is because the primary focus of modern clinical medicine has shifted from preventive public health intervention in infectious diseases to the cure and care of chronic diseases, cancers, organ transplants, and other high-tech medicine.6)
The People’s Action Party (PAP), the de facto Singapore government, has governed Singapore uninterruptedly since 1959, when Singapore attained self-rule. Singapore became an independent state in 1965. At the end of the 20th century, a report published by the WHO ranked Singapore 6th among 191 members under the category of “Health system performance in all Members States, WHO Indexes, estimates for 1997” (WHO 2000, 200). Key health indicators in 2009 were indeed impressive: Singapore’s infant mortality rate of 2.2 per 1,000 live births was one of the lowest in the world, and life expectancy at birth (male/female) stood at 79/83.7. The high economic development of Singapore today as well as its small land size (712.4 km2 as of 2010)—equivalent to that of Bahrain or Amami oshima of Japan—are often used to explain Singapore’s achievements in general.
The view that Singapore’s economic development and small size account for the country’s success in infectious disease management is too simplistic. Singapore has an environment suitable for the propagation of most pathogens. First, the island state is located 137 km north of the equator, and its tropical climate is characterized by high temperature and high humidity in addition to abundant rainfall. While Singapore is generally spared from natural disasters like earthquakes and tropical cyclones, it is the only industrialized nation situated in a tropical climate zone where infectious diseases are prevalent. Thus, Singapore faces far more health challenges than other developed societies. Second, the urban city-state faces further increase in population density. According to the Ministry of Trade & Industry, the total population was 1.9 million in 1965. The number increased to 5.08 million by the end of June 2010, composed of citizens (64 percent), permanent residents (11 percent), and others (25 percent).7) Whereas the overall population density was 7,022 persons per km2 in 2009, the central business district in the south central part of the main island is even more densely populated. More than 85 percent of the main island is already built up with residential, commercial, and industrial zones. Third, Singapore, identified as the financial, medical, and industrial hub in the region,8) experiences frequent movements of population. Although rural migration to urban areas within the country—typically seen in other urbanized areas in Southeast Asia—is absent, the movements of people in Singapore include not only students, tourists, business visitors, and foreign executives but also foreign migrant workers. These inherent conditions should not be underestimated.
As a result of frequent interactions between humans and pathogens in overcrowded urban areas, infectious diseases can be transmitted much easier in this tropical urban city-state than in less-populated rural areas. As long as Singapore desires to keep its national borders open to the global economy, importation of infectious diseases is inevitable. Referring to the period of the SARS outbreak, the then minister for national development stated that Singapore could not close its borders because of its role as “an international air hub and a major financial and business center” (Ministry of National Development 2003).
Focusing on etiology and clinical management, abundant scientific and medical research, e.g. by WHO (2003), has furthered the understanding of the new global health threat. The WHO (2006) not only provides details of the epidemiology, but also evaluates governmental responses of several countries and areas including Singapore. In the WHO’s 2006 publication, the Singapore government received good recognition: “Early cooperation from Singapore provided essential information that helped the global control of the SARS outbreak” ( ibid. , 106).
An objective evaluation of Singapore’s SARS containment measures from a political perspective is provided by Khai Leong Ho (2003) in an analysis of six Asian governments. Ho notes that others referred to Singapore’s policies and concludes that the country’s “right steps in the right directions” could stem from its “authoritarian” political environment, compact geographical size, and timeliness of actions. Chorh-Chuan Tan (2006) reviews achievements and shortcomings of Singapore’s measures and attributes the outbreak containment to “strong political leadership and effective command, control and coordination of responses.” On the other hand, Kai Khiun Liew (2006) blames the ruling party for “framing the containment of SARS in militaristic terms rather than as a public health issue” to “reinforce” political legitimacy. However, this condemnation can be challenged since words such as beat, defeat, and fight are commonly used when referring to actions to overcome diseases.
As for health policy formulation, Peggy Teo et al. (2005) present a compelling argument that decisions relying heavily on biomedical research alone could misplace social perspectives, pointing out possible “overpolicing” even among the historically compliant Singapore citizens. In contrast, legal implications of infectious disease management in Singapore are documented by Catherine Tay (2003), giving a good argument to support the legality of strict enforcement of public health measures.
Mui Hoong Chua (2004) expands the scope to observe the implementation and effects of Singapore’s measures in such areas as national cohesion, state actions, community reaction, and individual effort. A household survey in May 2003 revealed that more than 80 percent of respondents approved of official information and “authorities’ openness to communication” had a positive effect on compliance with preventive measures (Quah and Lee 2004). Another community survey conducted by Gabriel Leung et al. (2004) toward the end of the outbreaks found that Singapore respondents showed lower anxiety than residents in Hong Kong (HK).
Tan Tock Seng Hospital (TTSH) (2004) contributed its perspective on healthcare professionals and modern healthcare institutions in Singapore, recounting hardships during the SARS outbreak. Stronger evidence of the burden is reported by Kang Sim et al. (2004) and David Koh et al. (2005), revealing sufficient SARS-related psychiatric and posttrau-matic morbidity based on surveys conducted in healthcare settings in Singapore in July and mid-May to mid-July 2003, respectively.9)
Regarding overall public health measures, Kee Tai Goh et al. (2006) discuss initial weaknesses and improvements that were subsequently made, analyzing the epidemiology in hospitals, a laboratory, and communities in Singapore. Kee Tai Goh and Suok Kai Chew (2006) call for attention to EIDs by providing comprehensive accounts of the SARS transmissions, details of painstaking public health prevention and control measures, and the “framework” of SARS response in Singapore.
However, the existing scholarly research has not fully examined in detail the mechanism allowing the tiny nation to perform such a massive-scale infectious disease control nor explained why infectious diseases are recognized as important issues in the city-state. I will, therefore, analyze the emergency response of policy makers, public health policy implementation by health authorities, and involvement of local people. This analysis will involve public health perspectives and political, economic, and social issues. The result indicates that Singapore’s SARS management reflects the influence of political leaders. I will then show that this political will was present much earlier by tracing Singapore’s public health efforts to the first two decades immediately after the inception of the nation in 1965, when the country was susceptible to frequent outbreaks of classical infectious diseases. The measures implemented as national strategy earlier will reveal Singapore’s political determination to continue controlling infectious diseases. My hypothesis—that historically embedded political will ensures Singapore’s active governmental intervention in infectious diseases such as SARS—can then be tested.
II Methods and Materials
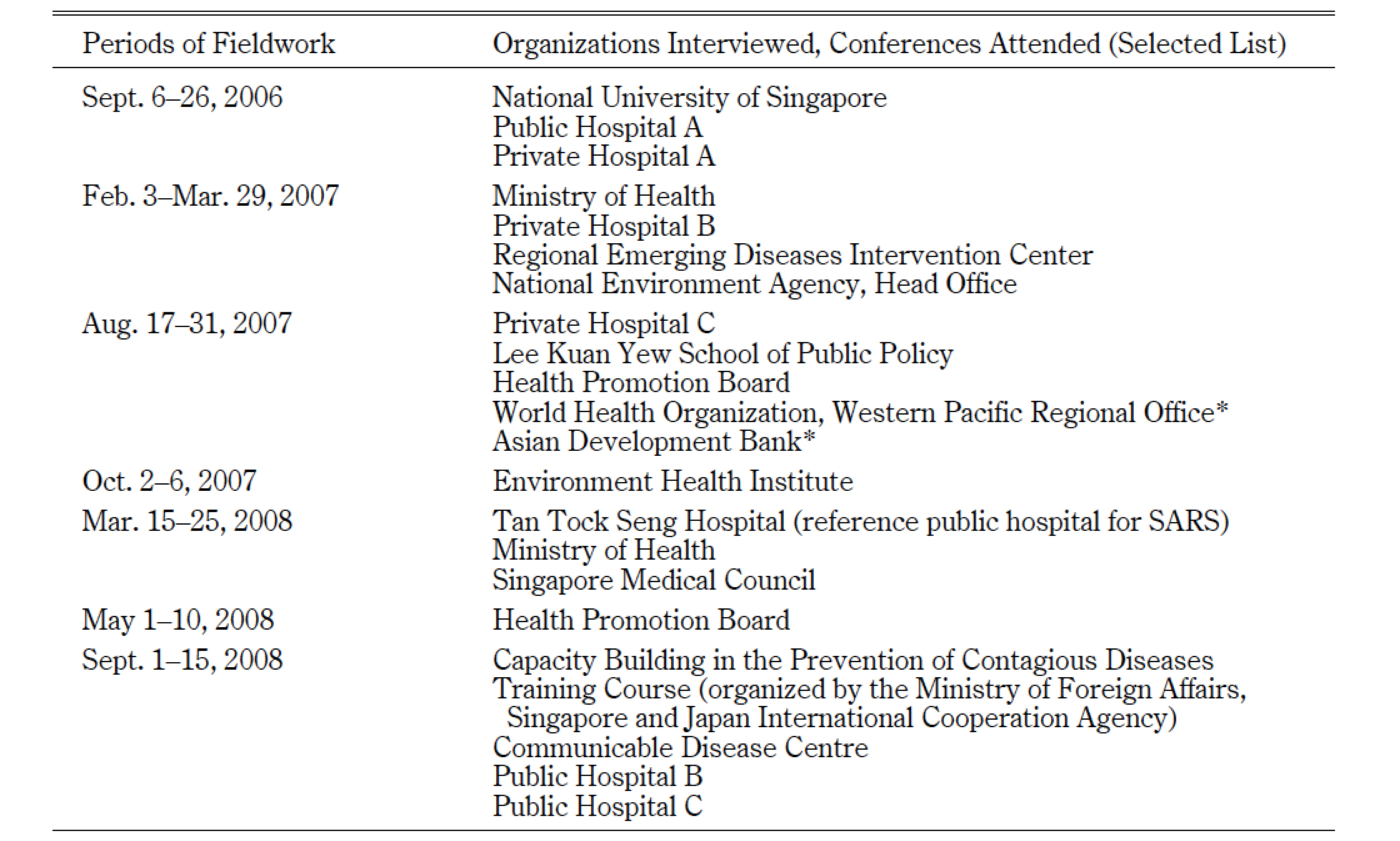
An area studies approach adopted in the present research combined literature investigation and extensive fieldwork in situ. Preliminary fieldwork was carried out in September 2006, when the feasibility of collecting information through interviews with civil servants, academics, scientists, healthcare providers, and other resource persons was confirmed. Subsequently, six fieldwork trips were conducted, mostly in Singapore, in 2007 and 2008, as shown in Table 1.
The fieldwork allowed access to governmental documents and local newspaper articles containing information from the 1960s to the 1980s. Interviews with health authorities at the Ministry of Health (MOH), its related organizations, and healthcare professionals displayed their hands-on approach in responding to the SARS outbreak and frequent references to the past struggle with infectious diseases. Furthermore, the fieldwork in Singapore generated favorable circumstances, i.e., direct observation and interaction with resource persons and other residents to evaluate how policies are actually implemented. It was beneficial to learn the views of international organizations toward the SARS threat and Singapore’s contribution in Manila in 2007. In addition, the author visited Singapore eight times between March 2009 and June 2011 (not listed in Table 1) for another research project, which provided opportunities to follow up this research. All field trips were funded by the Japan Society for the Promotion of Science and this author.
Table 1 Periods of Fieldwork, Major Organizations Visited, and Conferences Attended between 2006 and 2008
Note: * These are located in Manila, the Republic of the Philippines, while all others are in Singapore.
III Results: Singapore’s Anti-SARS Response
III-1 Being “UNIQUELY Singapore” 10) against SARS
“Atypical pneumonia” was the initial description of the disease that turned out later to be an extremely dangerous new infection. Most cases were caused by direct contact with infectious materials like respiratory secretions from a person with the disease; the incubation period ranged from 2 to 10 days. The etiological agent was subsequently identified as a new strain of coronavirus (CoV), and the microorganism was later named SARS-CoV. The EID was first imported into the city-state from HK by a Singaporean tourist who stayed at the Metropole Hotel, where the “super spreader” from the People’s Republic of China checked in on February 21, 2003, the beginning of annus horribilis. Literally one overnight stay of the symptomatic individual was enough for the lethal virus to infect as many as 16 hotel guests and one visitor.11) From here, the virus rapidly traveled to Canada, Vietnam, and Singapore along air routes. Patients initially complained of general symptoms like fever and cough, and SARS managed to deceive even ex perienced healthcare workers before developing into full-blown outbreaks at modern hospitals in urban cities like HK, Singapore, and Toronto, “bringing some public-health systems to their knees” (WHO 2006, vii).12) Soon, international trade stalled, tourism suffered, and stock markets plunged.
The prime minister of the Republic of Singapore at the time, Goh Chok Tong, took a very proactive role in the battle against SARS. On April 19, he conveyed the firm stance of the Singapore government to the people and asked for social responsibility from all Singaporeans at a media conference. This was followed by a parliamentary speech delivered on April 24 by the current Prime Minister Lee Hsien Loong, who was then the deputy prime minister and finance minister. He spoke about the three “battlefronts” that the government was determined to control: public health, economy, and society. He stressed the last as being the most “critical” and added: “Government is doing everything possible. But for these policies and measures to succeed, every Singaporean must play his part” (Chua 2004, 110). The political leaders uniquely pulled together politicians, civil servants, scientists,13) medical professionals, and the general public during the SARS outbreak. Singapore’s efforts to control SARS were praised by the WHO, who described it as “a 21st-century model for epidemic control,” referring to the effective public health measures and the careful plans of the government to promote support from the community (WHO 2006, 245).
The following five sections will investigate each of the distinctive areas in the containment of SARS in Singapore and show that the influencing forces boil down to a single factor: political will, which called for a total governmental approach.14)
III-2 Benefitting from the Rapid Response of Organizations and Groups
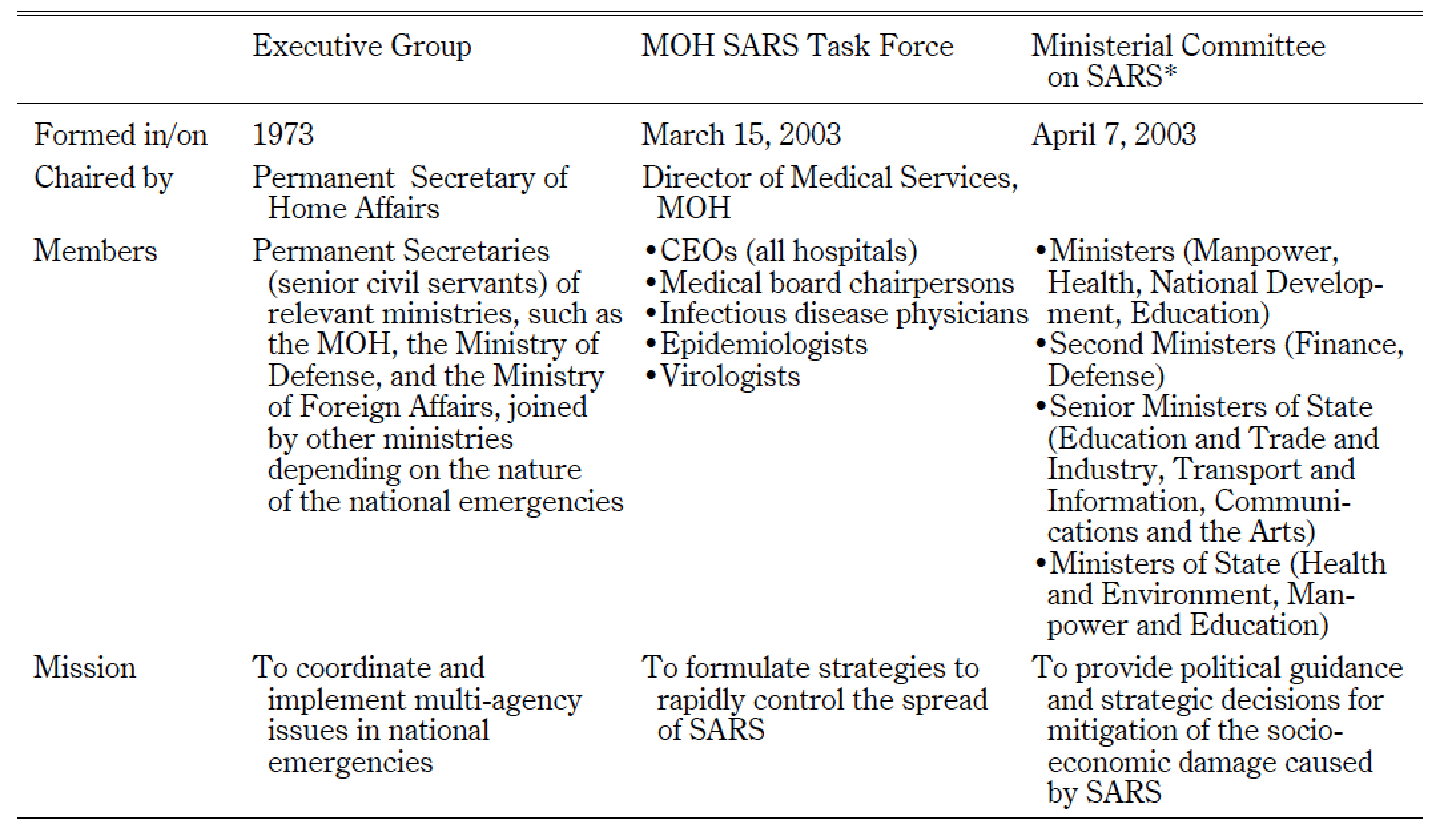
One of the notable features of Singapore’s SARS management was the quick mobilization of human resources that was enabled by the country’s organizations. Table 2 presents the major organizations that handled SARS management in Singapore. The MOH organ ized a task force only two days after Singapore learned about the first global alert on atypical pneumonia from the WHO. The government modified or added organizations to enhance its ability in making speedy decisions and implementing policies.
This flexibility is criticized by Michael Barr and Zlatko Skrbiš (2008), who judge that the government was incapable of controlling the SARS outbreak and that the response was “ad hoc and reactive” ( ibid. , 255). Being knowledgeable of Singapore’s health system but critical of the PAP’s rule, Barr dismisses Singapore’s SARS management as having been incapably stagnant for the first five weeks (Barr 2005, 168). This negative evaluation contradicts the findings by the majority of researchers, including those from the WHO, who have conducted numerous investigations into the microbiological, epidemiological and clinical features of SARS.
Table 2 Three Major Governmental Groups in Charge of SARS Management
Note: * Details are in a press release dated April 7, 2003, at http://www.mha.gov.sg/news_details.aspx?nid=ODI4-PvfDQeVER4s%3D, accessed August 7, 2011.
When problems went beyond the purview of medicine and the situation deteriorated globally, on April 7 Prime Ministry Goh Chok Tong established the Ministerial Committee on SARS, consisting of ministers (politicians) to strengthen the Executive Group of senior civil servants.15) The prime minister gave the committee a mission to provide policy opinions and strategic arrangements. His decision was a resolute step because the SARS management demanded a prescription that was different from previously known infectious diseases. For the cross-ministry coordination, the MOH in turn formed the Inter-Ministry SARS Operations Committee chaired by the ministry’s senior director of operations.
Referring to the works of Barr, Rodney King (2008) notes that “responsibility for handling the crisis was taken from the Minister for Health and then given to two ministerial committees” ( ibid. , 131). However, the health minister remained active in SARS management while non-clinical issues were coordinated by the committees. Singapore’s political leaders and public administration actually showed a unique concerted effort upon this pressing challenge.
The government effectively mobilized additional human resources in public services. An example was a flexible arrangement for the Ministry of Defence (MINDEF) and the Singapore Armed Forces (SAF) to assist the MOH with both physically labor-intensive and time-sensitive tasks requiring a strong chain of command.16) An army brigadier-general was seconded to the MOH to play a directive role such as conversion of vacant flats into quarantine quarters and large-scale contact tracing tasks. A statutory board under the MINDEF,17) the national authority on military technology and weapons known as the Defence Science & Technology Agency (DSTA), set up an IT system to trace diverse contacts. They ranged from healthcare providers, family members, visitors at healthcare institutions, school teachers, classmates, and workplace colleagues to commuters in close proximity to SARS cases (Goh et al. 2006, 302). Furthermore, the DSTA provided radio frequency identification tags for hospital infection control measures, which prevented accidental movements of healthcare providers beyond wards used for isolating SARS cases.
Another source enabling the dominant PAP to quickly mobilize resources was the People’s Association (PA). Established by the PAP in 1960, the PA is a statutory board chaired by the prime minister, and connects many grassroots organizations in Singapore with the government. Working with members of parliament, the PA functions to “strengthen racial harmony and social cohesion” and disseminates the government’s vision and common goals to the community.18) During the SARS outbreak, PA volunteers fluent in various Chinese dialects supported the English-speaking health officials. When the Singapore Civil Defence Force provided language assistance to individuals requiring translation during the contact tracing operations, 66 PA volunteers supported the task (Chua 2004, 81).19) Following the community outbreak at the Pasir Panjang wholesale vegetable center, the multilingual PA was mobilized jointly with the SAF and the police to rapidly cordon off the market. The PA volunteers administered fever checks in the community and distributed 1.1 million SARS kits consisting of thermometers, masks, and other items to every household ( ibid. , 123). Since SARS required an unprecedented scale and speed of mobilization of human resources, those in public services, the private sector, NGOs, schoolchildren, and volunteers responded.
Table 3 Highlights of Actions, Events, and Outcome in SARS-affected Developed Areas
Source: Modified from WHO (2006; 2007).
Note: 1) Date of removal differs among literatures; some sources like Chua (2004) state it as May 30.
2) (Taipei City Government 2005). Population of Taiwan was approximately 23 million.
3) It consists of 4.7 million in Greater Toronto area and 2 million in Vancouver out of 32 million in Canada.
In contrast, overconfidence and “the lack of broad general views of risk management” (Tambyah and Leung 2006, xxiii) could have contributed to the slower response in HK. The situation was made even more complicated by a concern that the novel disease might be due to the feared human-to-human transmitting H5N1 influenza. Table 3 shows that Singapore preceded not only HK but also Taiwan and Canada in isolation of probable cases and amendment of the law to include SARS as a legally notifiable disease. Singapore designated a SARS-dedicated hospital on March 22 and HK on March 26.20) The quicker actions of Singapore could partially explain the remarkable differences in outcome; the WHO removed Singapore from the list of SARS-affected areas on May 31, ahead of other locations, based on the condition for removal requiring the absence of new locally acquired cases for 20 days (Table 3). Singapore, with two-thirds the population of HK but one-seventh the number of patients and one-ninth the number of deaths, had a much smaller scale of spread. Following Vietnam, where foreigners initiated outbreak control, Singapore became the second country to contain the local transmission of SARS. The city-state “attracted a slew of very positive comments from even its most skeptical foreign critics” (Ho 2003, 196).
III-3 Preserving Consistency and Accuracy in Information Disclosure
As the Asian Development Bank recognized the magnitude of “isolation from the global community” of certain countries during the SARS period (Peralta and Hunt 2003, 79), a lack of transparency or insufficient information disclosure of health risks of global significance resulted in international condemnation. The People’s Republic of China was criticized for not having shared knowledge of new epidemic risks sooner, because the inaction delayed global awareness of the health peril. Although the government in China “was initially reluctant to disclose the gravity of the situation” (Fan and Chen 2007, 147), the newly sworn in President Hu Jintao and Premier Wen Jiabao replaced the mayor of Beijing and the minister of health, and demonstrated a dramatically different approach in disclosing the epidemic situation (Abraham 2007, 103).
In contrast, Singapore maintained constant communication with international communities. The WHO recalls that occasional telephone conversations with Singapore’s health minister enabled the agency to judge Singapore’s situation as unlikely to threaten the public health of the global community. This assessment led the WHO not to issue a travel advisory for Singapore (WHO 2006, ix) but to issue advisories for HK, Guangdong, Beijing, Shanxi, Toronto, Tianjin, Inner Mongolia, Taipei, and Hubei.
In addition, Singapore’s proactive information disclosure was uncompromised even when the MOH—observing the first global health alert three days earlier—communicated to the WHO soon after finding out that a potentially SARS-infected Singaporean physician was on a flight to Frankfurt. Singapore’s timely information was praiseworthy, as delayed action would have resulted in serious outcomes not only in Germany but also in many other parts of the world.
Initiating regular press releases and conferences, Singapore provided complete and timely information. However, biased foreign media information circulated. In response, the Ministry of Information, Communications and the Arts (MICA) engaged relevant agencies in monitoring and investigating reports, tracking down rumors, and verifying information (Chua 2004, 112). The Ministry of Home Affairs refuted an erroneous report in the Malaysian press (MHA 2003).
Furthermore, Singapore succeeded in mobilizing the local mass media to alleviate the fears of the public by airing updated information and educational messages. In other words, the mass media became effective tools of risk communication. On May 21, 2003, Singapore Press Holdings (a government-controlled press), Starhub (a telecommunications company), and Mediacorp (a media company) established the SARS TV channel, which streamlined SARS-related information by broadcasting programs in English, Mandarin, Malay, Tamil, and some Chinese dialects to capture as wide a viewership as possible (Chua 2004, 155–156).21) The print media disseminated educational materials prepared by government agencies such as the Health Promotion Board under the MOH. By and large, it can be said that the efforts at information disclosure demonstrated by the Singapore government won the praise of international health organizations and Singapore residents alike (Chan 2006, 361).
III-4 Rectifying Weaknesses of Healthcare Settings and Public Health Environment
Upon the emergence of SARS, the national referral center in charge of treating infectious diseases known as the Communicable Disease Centre (CDC) could not cope due to insufficient space.22) The CDC added 40 isolation rooms by May 7 and another 40 by May 17, and a new national center—CDC2—with 39 isolation and 18 ICU beds was constructed. Thus, the authorities improved healthcare infrastructure and capability with remarkable speed and magnitude. Three containment strategies, i.e., closure, ring fencing, and concentration of cases, were implemented at hospitals (Goh and Chew 2006, 294). TTSH no longer accepted other patients but became the designated SARS healthcare institution. The decision to centralize all SARS cases appears sensible, as it mitigated the risk of transmission in other healthcare settings.23)
The SARS-dedicated modern hospital suffered a few ill effects. The frequent transmission of the virus among healthcare professionals unveiled a gap in the use of N95 masks at TTSH (TTSH 2004, 24). The largest cluster of nosocomial, or hospital-acquired, transmission occurred among patients in the more crowded eight-bedded wards, reflecting cost pressure at modern hospitals. The SARS experience made the MOH stockpile up to six months’ worth of personal protective equipment supplies in preparation for surges in demand; and all other hospitals enhanced contingency plans (Goh and Chew 2006, 300–301). TTSH reduced the number of beds per ward to allow adequate distance among patients. Moreover, Singapore implemented a color-coded alert system that defined three levels of local transmission of infectious diseases and response protocols (MOH 2004, 1–5). This framework was applied for a pandemic influenza preparedness plan in Singapore (Goh et al. 2006, 311). Hence, the country’s competency in infectious disease management improved.24)
The government also saw it necessary to provide a safer environment to protect healthy individuals from SARS. The National Environment Agency (NEA) under the Ministry of Environment and Water Resources promoted a campaign emphasizing personal hygiene and environmental cleanliness. The NEA escalated many regular public services, e.g., cleaning and disinfecting public areas, culling pests, checking on waste disposal and collection, and inspecting sewerage systems.
A much more direct public health intervention, however, became necessary to disrupt the route of infection of SARS, which was transmitted from human to human. “When SARS emerged in Singapore in 2003 and contacts started to come down with the disease, my Minister for Health asked what could be done to prevent transmission. I suggested home quarantine but cautioned that it would be very difficult to enforce,” said Dr. Goh Kee Tai.25) After a few decades of absence of serious human-to-human transmissible infectious disease outbreaks, Singapore was not ready to implement the isolation procedure. Goh recalls the struggle: “we had to learn from scratch the operational problems of quarantining thousands of contacts during the outbreak.”26) In fact, the implementation of quarantine measures generated problems requiring active social management, which the next section will explain.
III-5 Addressing Social Issues with a Carrot-and-Stick Policy
The Environmental Public Health Act, which made littering or spitting in public places an offense, was already in effect before SARS struck Singapore. During the SARS outbreak, these offensive and irresponsible acts were considered anti-social due to their role in the spreading of germs (Tay 2003, 20). The MOH invoked the Infectious Diseases Act on March 24 and empowered health officers to carry out investigation, surveillance, and isolation. The mandatory Home Quarantine Order (HQO) was implemented by minis terial cooperation with the PA. The HQO required each person identified as having been in close contact with a SARS patient to stay at home for 10 days. The MOH hired officers (uniformed like police officers) from the government-linked security agency CISCO; the officers delivered HQOs and installed electronic surveillance cameras at the residences of quarantined individuals. Then, home surveillance personnel would telephone these individuals at random intervals daily to ask them to turn on and stand in front of the cameras. Offenders who violated the HQOs were monitored with electronic tags to make sure they stayed at home.27)
On top of strict laws and active persuasion by political leaders to ask residents to cooperate, the government provided social support to assist the individuals under the HQOs. The MOH sent nurses to provide medical advice. In addition, alternative premises were arranged for those who preferred to minimize disruption to other family members. An excursion to Jurong Bird Park, an aviary park, was arranged to cheer up families under quarantine. The Ministry of Community Development, Youth and Sports and the National Council of Social Service mobilized five welfare organizations to provide elderly care arrangements and counseling. PA volunteers delivered food to quarantined people. The government swiftly appointed Community Development Councils to administer an allowance scheme, which provided financial aid to those who had lost income due to HQOs.28) In total, more than 8,000 HQOs were issued (Tan 2006, 347). Although negative reaction to this intrusion of privacy was natural, a survey in Singapore showed as many as 93 percent of sampled individuals indicating a willingness to observe quarantine measures (Teo et al. 2005, 287).
However, a serious social problem soon surfaced. The quarantined individuals became feared as sources of infection. Lee Hsien Loong spoke against the discrimination and stigma on May 1, 2003; “[p]eople on HQOs are not dangerous, neither have they done anything wrong. It is just sheer bad luck that they came into contact with a SARS case. . . . They should not be feared or stigmatized” (MOH 2003).
Similarly, the general public came to avoid healthcare institutions and workers, potentially triggered by the approximately 76 percent of nosocomial cases in Singapore (WHO 2006, 189).29) “Being a TTSH nurse had quickly become a stigma in the public eye,” and some landlords asked nurses who worked for the hospital to move out (TTSH 2004, 116). The government soon responded: a hotline service for healthcare workers was established, and political leaders actively tried to influence the opinions of the people. Politicians delivered speeches urging the general public to show appreciation and express backing to healthcare professionals.
Soon, the Caring for SARS Caregivers project was initiated with the support of the Red Cross. Many healthcare workers in Singapore even volunteered to work in SARS wards. In contrast, wages had to be raised in Canada to retain staff, and 25 healthcare workers in Taiwan walked out in reaction to ring fencing of an affected hospital (Chua 2004, 186). A potential explanation for the outstanding dedication and professionalism displayed by healthcare workers in Singapore came from the former president of the Singapore Nurses Association: leadership-led elevation of healthcare professionals through media glorified their roles; social support provided by the government, such as accommodation arrangements, helped them concentrate and focus on their duties; and the younger nurses were especially motivated to overcome their fears and show courage.30)
III-6 Stimulating Economy by the Mobilization of Financial Resources
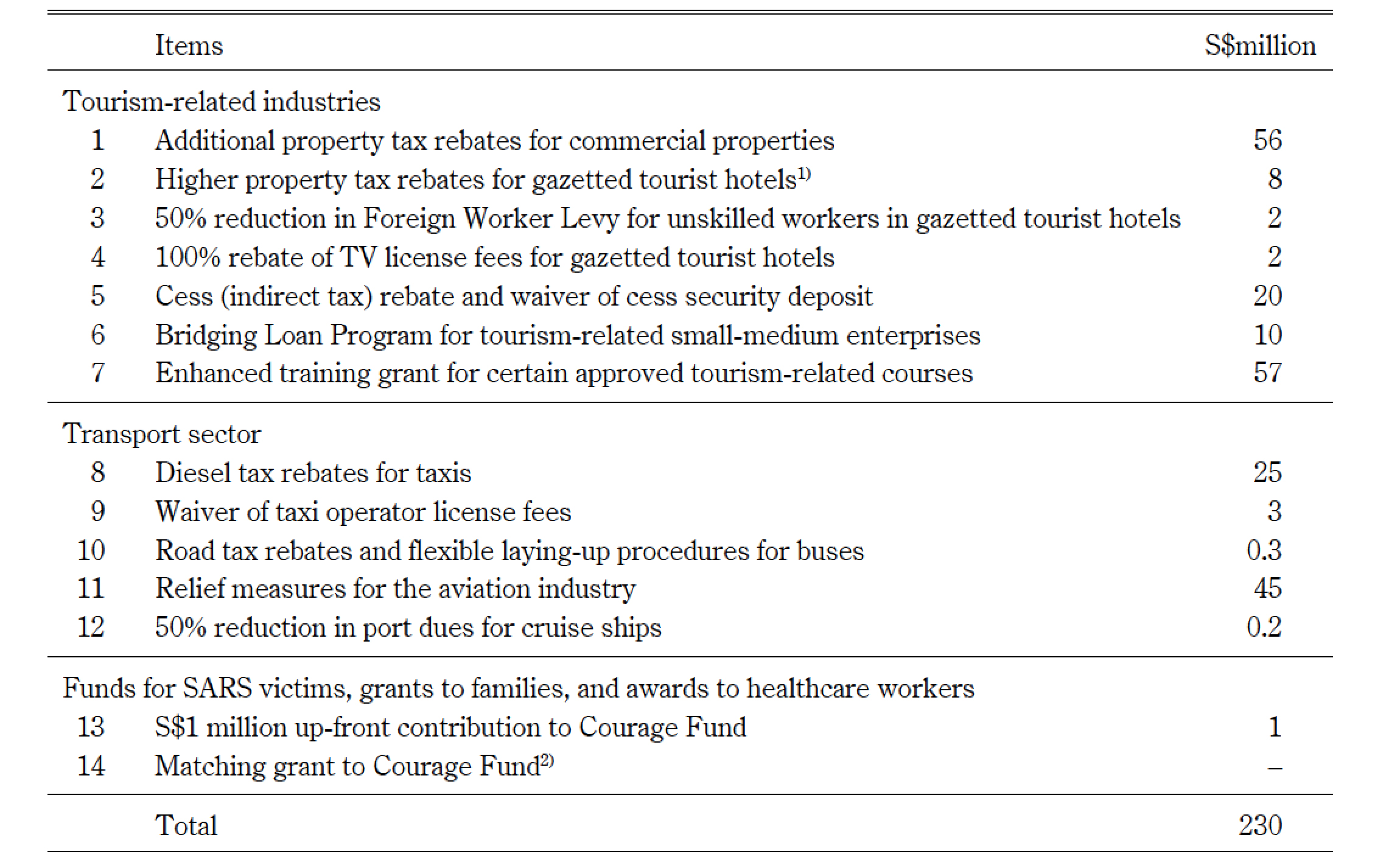
Despite the best efforts of the Singapore government, the epidemic still had a devastating economic impact. SARS inflicted damage on Singapore’s image as an attractive business and tourist destination. Although Singapore disclosed risk information and the WHO did not issue a travel advisory for the city-state, average hotel occupancy rates fell to 40 percent; inbound visitor arrivals dropped sharply, and retail, including restaurant sales, declined by the second quarter (Monetary Authority of Singapore (MAS) 2003, 10).31) Table 4 gives details of the S$230 million urgent financial relief package announced on April 17 by the government to rescue severely impacted industries such as the airline, cruise, hotel, and restaurant industries as well as affected individuals in taxi services and travel agents. As restoration of confidence in tourism was deemed necessary, the government set up an international image task force. Reportedly, foreign tour organizers were invited to Singapore to observe the tight control measures implemented at Changi International Airport. The decisiveness of the policy may have saved the macro economy from a much larger and more prolonged downturn.
Table 4 S$230 Million SARS Relief Package
Source: Modified from MAS (2003, 15).
Note: 1) Gazetted tourist hotels are premises declared under the Singapore Tourism Act.
2) Other measures except for this item ended by December 31, 2003.
IV Discussion
The previous section described examples of challenges faced and measures implemented by the Singapore government in response to SARS. Singapore’s massive and wide range of reactions to SARS prompts the question as to why the city-state takes such an aggressive stance in defending against EIDs. In addition to SARS, the Singapore government is also active and persistent in fighting against mosquito-borne infectious diseases such as dengue virus infection and chikungunya fever.32) In this section, I will discuss the motivation behind the Singapore government’s desire to control infectious diseases and show that this political will has been exercised over decades. It appears that the seemingly overreactive measures have their roots in the core values or strategies selected by the first generation of political leaders at the birth of the nation, when controlling infectious diseases was not an option but a necessity.
IV-1 Singapore’s Aim to Become a Global City
“History teaches that the improvement of human health at the population level is largely determined by good policies . . . ” (Peralta and Hunt 2003, 1).
Singapore’s encounter with infectious diseases dates back to the days when the territory was a former British colonial trading port. During the colonization, migrant workers especially suffered from a wide range of diseases. Singapore saw smallpox, plague, diphtheria, cholera, and malaria in the early 20th century; typhoid in the 1930s; polio in the 1940s and 1958; and Asian influenza in 1957 (Chan and Ting 2007, 8–10).
Singapore joined the Federation of Malaysia on August 31, 1963, and was expelled from the federation two years later. The Republic of Singapore was born on August 9, 1965. The loss of an important hinterland presented new challenges, and the young nation was required to alter policies. The new country was full of people to feed but had few natural resources, insufficient agricultural products, a sluggish economy, and no particular industry.33) Under the backdrop of 10 percent unemployment in Singapore in the 1960s (Trocki 2006, 148),34) President Sukarno’s Confrontation Policy in Indonesia, and the need to keep a distance from the communist-ruled People’s Republic of China, three issues haunted Lee Kuan Yew, Singapore’s prime minister from 1959 to 1990. These issues were international recognition, defense, and the economy (Lee 2000, 22–23). The overnight S$157 million loss due to the devaluation of the sterling pound in November 1967 (Tan 2007, 137),35) and the British withdrawal from Singapore, deprived the new nation of 70,000 service jobs (Lee 2000, 69). Chong-Yah Lee calculated the impact as 15–16 percent of gross national product between 1968 and 1971 (Lee 1980, 4, 41). Thus, pessimism prevailed: “Economically and politically separate from Malaysia, militarily separate from the UK, not many would have predicted the economic success and political stability . . . ” (Trocki 2006, 127).
Under these delicate geopolitical and challenging economic circumstances, PAP leaders like Lee Kuan Yew and Goh Keng Swee, “the architect of Singapore’s economy,” chose a strategy of inviting foreign direct investment (FDI) and multinational corporations (MNCs) to develop industries.36) The new government, with the assistance of the Economic Development Board (established in 1961 by the PAP), approached the United States, Japan, Europe, and the Commonwealth while keeping reasonably good relationships with the former suzerain ( ibid. , 127–128).37) The newly independent state thus became destined to survive as a “Global City” by opening the country wide to the world.38)
The Global City concept was introduced in 1972 by Sinnathamby Rajaratnam, who is best remembered as a minister for foreign affairs. He expected Singapore to become an advanced city, connected through cable, satellite, international financial networks, air, and sea, catering to both regional and global destinations. He conceptualized that Singapore’s survival would benefit from “a relationship of interdependence in the rapidly expanding global economic system” (Kwa 2006, 165–179). Political will was exercised by the first generation of Singaporean leaders in choosing the national strategy of a Global City to feed the people, bring prosperity, and sustain the nation. Achieving the goal, however, required multiple tasks, i.e., govern mental actions, in the newly born country.
Several components of Singapore’s industrialization strategy are well understood, including its legal system, tax incentives, and wage management. However, the mechanisms of the vigilant control of infectious diseases—which have resulted in the improvement of population health—remain insufficiently understood.39) Population health is an important factor for MNCs when evaluating investment risks. While an acute “health shock” can quickly impact capital markets as seriously as a coup d’état or the assassination of an important politician, FDIs react more slowly. Nevertheless, these long-term investors are likely to link unhealthy citizens to system failure or the incapability of policy makers (Tandon 2005, 1–3). In other words, a government must first respond to problems of a public health nature. Japan is a good example of this concept: there is a popular belief that Japan’s economic progress led to the successful control of infectious diseases, but in fact, its GNP rose sharply only after roundworm prevalence was lowered from 60 to 5 percent and schistosomiasis from nearly 15 to 2 to 1 percent in the early 1960s (Takeuchi 2004, 177–179).
Since shortages in manpower in addition to scarcity of land could have been fatally disadvantageous for Singapore’s budding development, ensuring the health of the labor force became an essential prerequisite for the Singapore government, which required FDIs to build up industries, create jobs, and generate production. Leaders saw it as their responsibility to furnish citizens with a solid structure in which they could “learn, work hard, be productive and be rewarded accordingly” (Lee 1998, 132). Visualizing Singapore’s transformation into “the cleanest and healthiest state in Asia,”40) the Lee Administration began improving social services. As Kai Lok Chan (1985) notes, referring to the urban slum conditions in the mid-1960s (ibid. , 56),41) a series of housing policies followed along with education and healthcare services. Chairman of the Housing Development Board (HDB) Lim Kim San, now popularly referred to as “Mr. HDB,” became minister for national development in 1963 and announced the Home Ownership Scheme in 1964. The board started providing low-cost public housing to the low-income segment of the population (Turnbull 1982, 316), amounting to 105,420 apartments between 1966 and 1975 alone, thus increasing the percentage of total population living in public units from 24 to 54.8 percent (Chan 1985, 57). The housing policy contributed to the improvement in living conditions of those who had previously lived in slums.42)
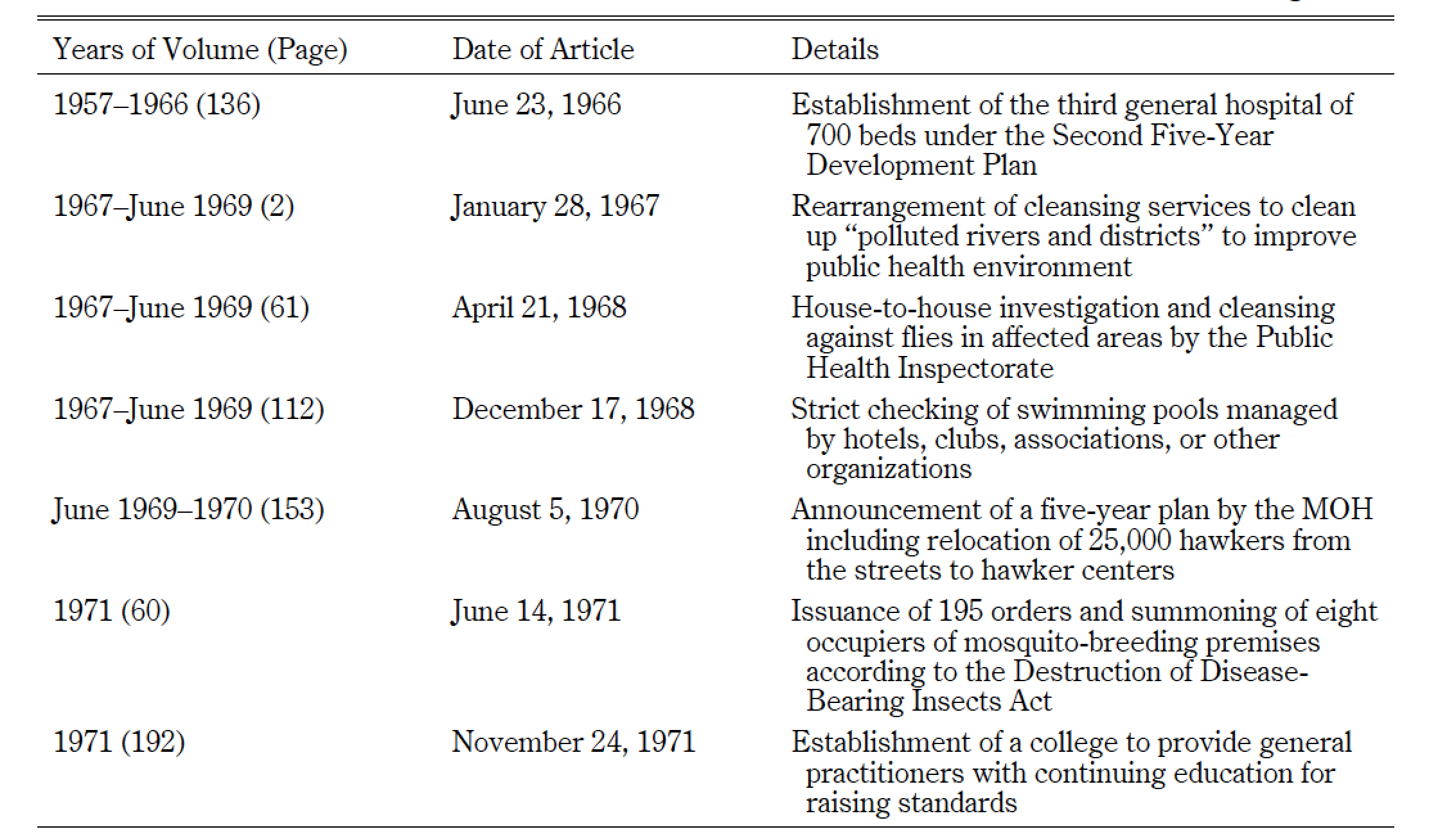
Indeed, painstaking efforts were made to improve population health across the nation.43) My data collection from the English language newspaper the Straits Times ( ST) confirmed ample evidence of infectious diseases and the determination with which the Singapore government acted in the 1960s and 1970s. Table 5 shows examples of these actions, with the five-year plan announced by the minister of health in 1970 declaring “[g]overnment’s effort of providing a better and healthier environment for the people to live in.”44) The country had neither sufficient healthcare providers nor facilities.45) In response, the government encouraged the local medical education system to produce more Singaporean doctors while at the same time ensuring sufficient doctor numbers by recruiting foreign doctors. Five hospitals were built between 1960 and 1974; 13 outpatient dispensaries in 1959 was doubled to 26 in 1974 (Barr 2005, 148). As a result, there was one physician for every 1,404 people in 1971, an improvement from 1,968 people in 1966.46)
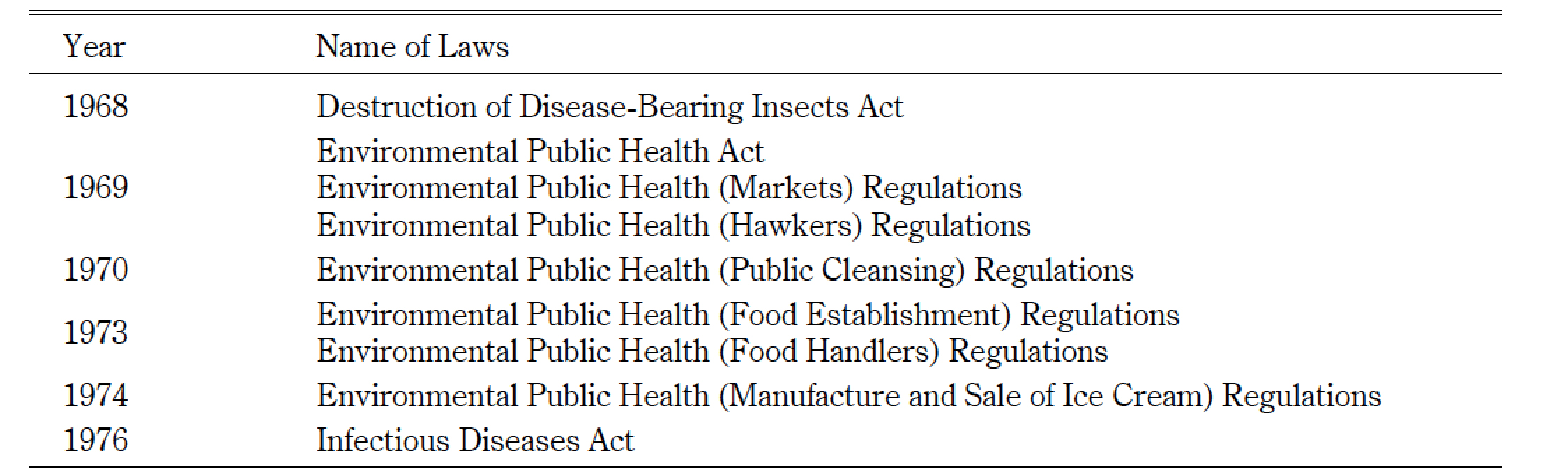
Outbreaks of cholera and typhoid occurred almost every year in the early years. In the year of independence, less than 80 percent of about 50,000 street hawkers involved in food services were licensed and knowledgeable about public hygiene, and these hawkers consequently attracted flies and rats (National Archives of Singapore 2008, 27). Intensive investigations of food-borne infectious diseases indeed often traced the route of transmission to those engaged in food services at local hawker centers and schools (Singapore Government 1967, 308). In response, the Health Ministry occasionally issued warnings and introduced regulations to food handlers in the Hawkers Code in 1965.47) Table 6 summarizes public health-related laws. For example, The Environmental Public Health Act in 1969 made it illegal for premise occupiers not to “dispose of refuse or filth within 48 hours” and for anyone to litter in public places.
After its inauguration in September 1972, the new Ministry of the Environment took over the responsibility for environmental public health from the MOH, including vector control, food hygiene, and sanitation.48) In October 1973, both ministries formed the Joint Coordinating Committee on Epidemic Diseases, joined by the National University of Singapore, the MINDEF, and the Ministry of National Development. A series of public persuasion campaigns was used to change collective and individual habits like littering, spitting, and smoking to improve the public environment (Liew 2006, 374–375).49) In 1976, the Ministry of Education supported the MOH in promoting the National Health Campaign to fight against infectious diseases. The coordination across ministries and sectors in addition to campaign-based health education efforts characterizes Singapore’s infectious disease management even today.
Table 5 Details of Health-related Governmental Actions from the Straits Times Press Cuttings
Source: NUS (1957–66; 1967–June 1969; 1971).
In 1965, the infant mortality rate was 26.3 per 1,000 live births and life expectancy at birth was 64.5 years. These figures had improved to 7.6 and 73.9 respectively by 1985 (MTI 2007, 63). The city-state has so far attracted MNCs in various successful industries.50) The GDP increased from S$2.1 billion in 1961 to S$55.3 billion in 1989 (De Koninck et al. 2008, 42). It can be said that the strong political leadership and governmental efforts at the nascence of the state enabled a country with few natural resources to establish a good health system, which in part facilitated the investments from FDIs. While it is difficult to quantify, the health of Singaporean citizens may have contributed to the economic growth.51)
Table 6 Laws to Control Infectious Diseases Introduced/Amended by the Government in the First 11 Years
Source: Constructed from National Archives of Singapore (2008, 118) and Goh (1983).
IV-2 Singapore’s Determination to Remain Open to the World
By the 1980s, Singapore had achieved good control of general infectious diseases under the leadership of the first generation of political leaders. The baton was passed to the next-generation leader Goh Chok Tong and his administration.52) Under Lee Kuan Yew, Goh had already demonstrated his dedication to public health by introducing the National Health Plan in 1983, introducing medical savings accounts, and restructuring the government hospital program. He believed that his people must be “physically fit, mentally tough, healthy, skilled, well-educated and economically productive” (Goh 1982, 84). Indeed, Goh “viewed social investments in health, education and housing as prerequisites to happiness and progress” (Phua 2009, 253–264).
Singapore’s inherent “optimal conditions” for pathogens (Goh 1983, ix) remain. These conditions are attributable to area-specific factors such as geographic location and an economy reliant on trade. In a pandemic situation, EIDs might reach trading hubs sooner (Lee et al. 2007, 1056). Since the 1990s, the Global City has seen Bengal cholera, multi-drug-resistant salmonellosis, norovirus gastroenteritis, Nipah virus infection, meningococcal disease, and hand-foot-and-mouth disease (Goh et al. 2006, 301).53) SARS clearly tested the leadership skills of the second generation of political leaders in infectious disease management. We have seen Singapore’s renewed determination to fight against the health threats not only nationally but also regionally. Singapore proposed that health ministers discuss regional cooperation to control SARS at the ASEAN Summit in Bangkok in April 2003 (Phua 2009, 262–263). In light of the transnational nature of EIDs, Prime Minister Goh agreed to jointly establish the Regional Emerging Diseases Intervention Center in Singapore with the United States.
To understand why public health management of EIDs is a problem of national importance in Singapore, it is important to stress that Singapore’s compact geographical size does not guarantee successful containment of infectious diseases. The seemingly advantageous smallness could rather be a disadvantage; it exposes a large portion of the country at once when a deadly epidemic takes place, as there are few alternative spaces to relocate uninfected individuals. To make matters worse, the tiny population size suggests that high prevalence could easily cause dysfunction in the country’s system. Hence, Singapore has little margin for error. The high population density and people’s movements in Singapore point to serious consequences in population health, economy, and society if the country fails to control EIDs. Therefore, the government is aware of the very high cost of inaction. This conviction could result in governmental intervention in infectious diseases that may sometimes seem aggressive or draconian.
In August 2004, Goh was succeeded by Lee Hsien Loong, who had played a vital role under the Goh Cabinet during the SARS outbreak, as described earlier. Although public health intervention in the transmission of EIDs often requires forceful measures, it is becoming more difficult to impose intrusions of privacy, especially in developed areas today. In Singapore, there are at least two area-specific difficulties that the current leadership may face. The first difficulty refers to the election on May 7, 2011. The ruling PAP not only lost the Aljunied Group Representation Constituency to the Workers’ Party but also suffered from a declined share of votes—from 66.6 percent in 2006 to 60.1 percent.54) The issues with which the general public has expressed unhappiness seem to include: styles of public decision-making, reduced interaction between the government and citizens, and the perceived socioeconomic class privilege of foreign executives.55) Singapore might be finding it difficult to cope with its own economic achievements, which have been realized too fast. The second difficulty is the demography of populations. Only 64 percent of Singapore’s population is composed of citizens, and there is a large influx of foreign workers and visitors. Securing sympathy toward the importance of public health intervention may become even more challenging for the government. Should there be any future serious threats to the city-state, implementation of strict infectious disease control and solicitation of public support could become a more challenging task for Singapore.
There are several limitations to this study. Historical reviews were largely concentrated in the first two decades of independence, and the relationship between healthy labor and FDI could not be quantified conclusively. The political will of the current administration to control EIDs has yet to be substantiated. However, we can see Singapore’s increasing international contribution in EID management, especially after the SARS ordeal. For example, a week-long training program was jointly sponsored by Singapore’s Ministry of Foreign Affairs and Japan International Cooperation Agency in 2008. I personally observed experts in infectious disease control from Singapore enthu-siastically explain the experiences of SARS and plans against H5N1 influenza to participants from seven ASEAN countries.56)
V Conclusion
The previously unknown SARS suddenly required Singapore to prescribe a panacea. This paper scrutinized tools utilized by the city-state, and elucidated the important role of the Singapore government in promoting and supporting the public health measures. The determination of political leaders to control the SARS outbreak was demonstrated through the total governmental approach. It involved top political leaders, ministers, and public servants, and initiated public-private cooperation. The mechanism enabling the compact country to carry out grand and quick public health measures included government-linked Singapore-style grassroots organizations, which played vital roles in rapidly deploying the rather scarce human resources of the country. In addition, the government adhered to timely and accurate information disclosure. It also facilitated improvements of healthcare settings and environmental health. To implement strict measures such as home quarantines, the government rapidly enacted or revised laws to enable the authorities to enforce the measure, supplied facilities within a short time, and provided necessary public health, social, and financial support to the quarantined people. Political leaders preempted socially destructive stigma against healthcare workers, patients, and quarantined individuals before it became out of control, and relieved the significant part of economic damage. All of these measures point to Singapore’s uncompromising political will that enabled the formulation and implementation of strategies to control SARS. Hence, Singapore’s prescription revealed one factor that was different from economic prosperity or compact territorial size.
This paper also argued that Singapore’s past health policy, including vigilant infectious disease control, has promoted population health, which has in turn likely contributed to economic and trade activities in the two decades following the country’s independence. Bringing health to citizens and transforming Singapore into an attractive place were prerequisites for the first generation of political leaders to invite FDIs, which subsequently contributed to securing survival and prosperity for Singapore. Therefore, it can be said that Singapore is a country that has realized the national importance of containing infectious diseases from early in its history.
The quick control of SARS in Singapore depicts the national stance of making it a priority to defend the nation’s competitiveness in the international market. The mission to continue fighting against EIDs is never more applicable to any other countries than Singapore because the Republic is one of the most trade-dependent nations. Active governmental intervention in infectious disease control might depend on how high the respective government places the issue of EIDs in the agenda, i.e., whether or not leaders prioritize responsibilities in solving public health problems. The data presented in this paper are consistent with the hypothesis that active governmental intervention in the SARS outbreak was ensured by the historically embedded political will in the Re public of Singapore. The understanding of the fatal connection between the emergence of public health threats and damage to national viability prompted political leaders in Singapore to persuade the general public to work with the government and play a part in maintaining a good public health environment. This paper documented the country’s irreversible commitment to drive away public health threats.
Acknowledgements
This research was supported in part by Grant-in Aid for Scientific Research (KAKENHI 19101010 and 19251005) and Initiatives for Attractive Education in Graduate Schools by the Japan Society for the Promotion of Science. I would like to thank Dr. Phua Kai Hong from the Lee Kuan Yew School of Public Policy for his insights into health policy and kind introduction to valuable contacts, including Dr. Goh Kee Tai and Dr. Chew Suok Kai—both from the Singapore Ministry of Health—who graciously helped me clarify essential information. I am grateful to Dr. Chee Heng Leng at Asia Research Institute, the National University of Singapore, who arranged for me to use the resources of the university’s libraries. Special mention should be made of all who willingly spent time with me during my fieldwork in Singapore.
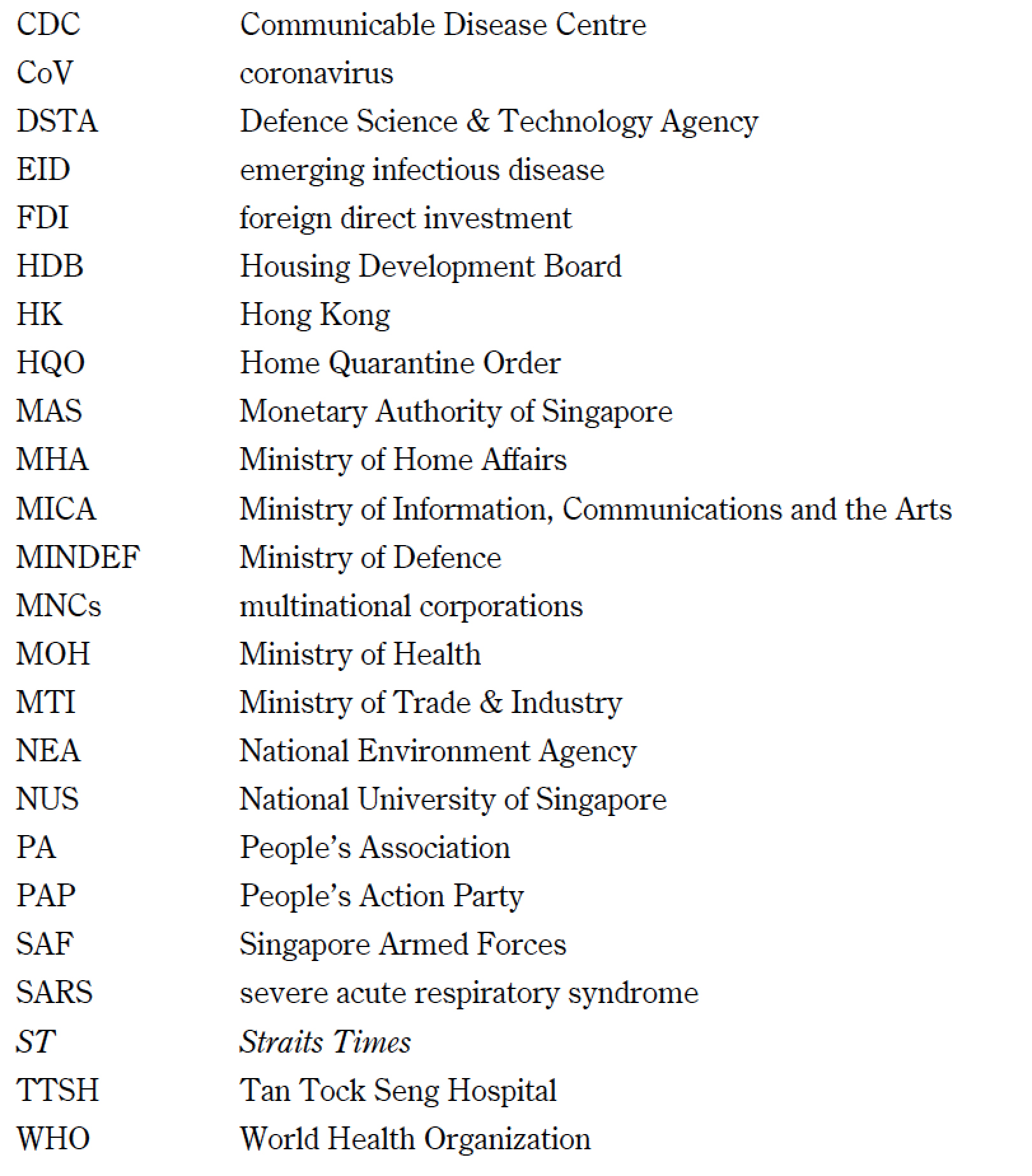
List of Abbreviations
References
Abraham, Thomas. 2007. Twenty-First Century Plague: The Story of SARS. Baltimore: The John Hopkins University Press.
Acharya, Amitav. 2008. Singapore’s Foreign Policy: The Search for Regional Order. Singapore: World Scientific.
Barr, Michael. 2005. Singapore. In Comparative Health Policy in the Asia-Pacific, edited by Gauld Robin, pp. 146–173. Berkshire: Open University Press.
Barr, Michael D.; and Skrbiš, Zlatko. 2008. Constructing Singapore: Elitism, Ethnicity and the Nation-Building Project. Copenhagen: NIAS Press.
Chan, C. K. 2006. Risk Perception and Coping Responses in a SARS Outbreak in Malaysia. In Population Dynamics and Infectious Diseases in Asia, edited by A. C. Sleigh, H. L. Chee, B. S. Yeoh, K. H. Phua, and R. Safman, pp. 351–368. Singapore: World Scientific.
Chan, John; and Ting, Yuanyi. 2007. The CDC Story: Historical Accomplishments & Challenges 1907–2007. Singapore: Communicable Disease Centre.
Chan, Kai Lok. 1985. Singapore’s Dengue Haemorrhagic Fever Control Programme: A Case Study on the Successful Control of Aedes Aegypti and Aedes Albopictus Using Mainly Environmental Measures as a Part of Integrated Vector Control. Tokyo: Southeast Asian Medical Information Center.
Chua, Mui Hoong. 2004. A Defining Moment: How Singapore Beat SARS. Singapore: Institute of Policy Studies.
Da Cunha, Derek, ed. 2002. Singapore in the New Millennium: Challenges Facing the City-State. Singapore: Institute of Southeast Asian Studies.
De Koninck, Rodolphe; Drolet, Julie; and Girard, Marc. 2008. Singapore: An Atlas of Perpetual Territorial Transformation. Singapore: NUS Press.
Dobbs, Stephen. 2003. The Singapore River: A Social History 1819–2002. Singapore: Singapore University Press.
Fan, Yun; and Chen, Ming-chi. 2007. The Weakness of a Post-authoritarian Democratic Society: Reflections upon Taiwan’s Societal Crisis during the SARS Outbreak. In SARS: Reception and Inter pretation in Three Chinese Cities, edited by Deborah Davis and Helen Siu, pp. 146–164. Oxon: Routledge.
Ganesan, N. 2002. Governance: Its Complexity and Evolution. In Singapore in the New Millennium: Challenges Facing the City-State, edited by Derek Da Cunha, pp. 50–68. Singapore: Institute of Southeast Asian Studies.
Goh, Chok Tong. 1982. Stay Well for Health. In Our Heritage and Beyond, edited by S. Jayakumar, pp. 82–86. Singapore: Singapore National Trades Union Congress.
Goh, Kee Tai. 1983. Epidemiological Surveillance of Communicable Diseases in Singapore. Tokyo: Southeast Asian Medical Information Center.
Goh, Kee Tai; and Chew, Suok Kai. 2006. Epidemiology of Emerging Infectious Diseases in Singapore, with Special Reference to SARS. In Population Dynamics and Infectious Diseases in Asia, edited by A. C. Sleigh et al. , pp. 287–304. Singapore: World Scientific.
Goh, Kee Tai; Cutter, Jeffery; Heng, Bee-Hoon; Ma, Stefan; Koh, Benjamin K. W.; Kwok, Cynthia; Toh, Cheong-Mui; and Chew, Suok-Kai. 2006. Epidemiology and Control of SARS in Singapore. Annals Academy of Medicine 35(5): 301–316.
Han, Fook Kwang; Ibrahim, Zuraidah; Chua, Mui Hoong; Lim, Lydia; Low, Ignatius; Lin, Rachel; and Chan, Robin. 2011. Lee Kuan Yew: Hard Truths to Keep Singapore Going. Singapore: Straits Times Press.
Ho, Khai Leong. 2003. SARS, Policy-making and Lesson-drawing. In The New Global Threat: Severe Acute Respiratory Syndrome and Its Impacts, edited by Koh Tommy, Aileen Plant, and Eng Hin Lee, pp. 195–207. Singapore: World Scientific.
King, Rodney. 2008. The Singapore Miracle, Myth and Reality. Second Edition. Inglewood: Insight Press.
Koh, David; Lim, Meng Kin; Chia, Sin Eng; Meng, Ko Soo; Qian, Feng; Ng, Vivian; Tan, Ban Hock; Wong, Kok Seng; Chew, Wuen Ming; Tang, Hui Kheng; Ng, Winston; Muttakin, Zainal; Emmanuel, Shanta; Fong, Ngan Phoon; Koh, Gerald; Kwa, Chong Teck; Tan, Keson Beng-Choon; and Fones, Calvin. 2005. Risk Perception and Impact of Severe Acute Respiratory Syndrome (SARS) on Work and Personal Lives of Healthcare Workers in Singapore: What Can We Learn? Medical Care 43(7): 676–682.
Kwa, Chong Guan. 2006. Writing Singapore’s History: From City-State to Global City. In S Rajaratnam on Singapore: From Ideas to Reality, edited by Chong Guan Kwa, pp. 165–179. Singapore: World Scientific.
―. 2002. Relating to the World: Images, Metaphors, and Analogies. In Singapore in the New Millennium: Changes Facing the City-State, edited by Derek Da Cunha, pp. 108–132. Singapore: Institute of Southeast Asian Studies.
Lee, Chong-Yah. 1980. Economic Development in Singapore. Singapore: Federal Publications.
Lee, Edwin. 2008. Singapore: The Unexpected Nation. Singapore: Institute of Southeast Asian Studies.
Lee, Kuan Yew. 2000. From Third World to First: The Singapore Story: 1965–2000. Singapore: Times Media.
―. 1998. The Singapore Story. Singapore: Times Editions.
Lee, Vernon J.; Chen, Mark I.; Chan, Siew Pang; Wong, Chia Siong; Cutter, Jeffery; and Goh, Kee Tai. 2007. Influenza Pandemics in Singapore, a Tropical, Globally Connected City. Emerging Infectious Diseases 13(7): 1052–1057.
Leung, Gabriel M.; Quah, Stella; Ho, Lai-Ming; Ho, Sai-Yin; Hedley, Anthony J.; Lee, Hin-Peng; and Lam, Tai-Hing. 2004. A Tale of Two Cities: Community Psychobehavioral Surveillance and Related Impact on Outbreak Control in Hong Kong and Singapore during the Severe Acute Respiratory Syndrome Epidemic. Infection Control and Hospital Epidemiology 25(12): 1033–1041.
Liew, Kai Khiun. 2006. A Defining Moment, Defining a Moment: Making SARS History in Singapore. In Population Dynamics and Infectious Diseases in Asia, edited by A. C. Sleigh et al. , pp. 369–388. Singapore: World Scientific.
Machida, Kazuhiko 町田和彦. 2005. Kansensho Warudo: Menekiryoku, Kenko, Kankyo 感染症ワールド―免疫力・健康・環境[World of infectious diseases: Immunity, health, environment]. Tokyo: Waseda University Press.
National Archives of Singapore. 2008. 10 Years that Shaped a Nation. Singapore: National Archives of Singapore.
National University of Singapore (NUS). 1957–81 (various years). Medical and Health Services in Singapore (Straits Times Press Cuttings). Singapore: Central Library, National University of Singapore.
Peralta, Genandrialine L.; and Hunt, Joseph Michael. 2003. A Primer of Health Impacts of Development Programs. Manila: Asian Development Bank.
Phua, D. H.; Tang, H. K.; and Tham, K. Y. 2005. Coping Responses of Emergency Physicians and Nurses to the 2003 Severe Acute Respiratory Syndrome Outbreak. Academic Emergency Medicine 12(4): 322–328.
Phua, Kai Hong. 2009. Prescribing New Economic Medicine for Healthcare. In Impressions of the Goh Chok Tong Years in Singapore, edited by Bridget Welsh, James Chin, Arun Mahizhnan, and Tan Tarn How, pp. 252–264. Singapore: NUS Press.
―. 1989. The Development of Health Services in the Colonies: A Study of British Malaya and Singapore. Asia-Pacific Journal of Public Health 3(4): 315–323.
Quah, Stella R.; and Lee, Hin-Peng. 2004. Crisis Prevention and Management during SARS Outbreak, Singapore. Emerging Infectious Diseases 10(2): 364–368.
Republic of China (Taiwan), Taipei City Government. 2005. Yearbook 2004. http://yearbook.taipei.gov.tw/ct.asp?xItem=1001483&ctNode=21065&mp=100057, accessed July 3, 2011.
Sim, Kang; Chong, Phui Nah; Chan, Yiong Huak; and Soon, Winnie Shok Wen. 2004. Severe Acute Respiratory Syndrome-Related Psychiatric and Posttraumatic Morbidities and Coping Responses in Medical Staff within a Primary Health Care Setting in Singapore. Clinical Psychiatry 65(8): 1120–1127.
Singapore, Singapore Government. 1967. Singapore Year Book 1965. Singapore: Authority Government Printing Office Singapore.
Singapore, Ministry of Health (MOH). 2004. Singapore’s Preparedness to Deal with Possible Northern Winter Resurgence of SARS. Epidemiological News Bulletin 30(1) (January): 1–5.
―. 2003. SARS: A National Response. Speech at Parliament by Mr. Lee Hsian Loong, Deputy Prime Minister, April 24, 2003.http://www.moh.gov.sg/mohcorp/speeches.aspx?id=17009, accessed July 3, 2011.
―. 1968. Report of the Ministry of Health for the Year Ended December 1965. Singapore: Ministry of Health.
Singapore, Ministry of Home Affairs (MHA). 2003. Cases Reported by Malaysian Press on Persons Said to Have Caught SARS from Singapore. Press Release, May 27, 2003. http://www.mha.gov.sg/news_details.aspx?nid=NzY0-GMTDQLBwVhw%3d, accessed July 3, 2011.
Singapore, Ministry of National Development. 2003. SARS: Responding to A Lethal Threat. Keynote Address by Mr Mah Bow Tan, Minister for National Development to 33rd ISC-Symposium, May 24, 2003, also available at Text Archival and Retrieval System of National Archives of Singapore, document number 2003052401.
Singapore, Ministry of Trade & Industry (MTI). 2007. Singapore 2007 Statistical Highlights. Singapore: Singapore Department of Statistics.
Singapore, Monetary Authority of Singapore (MAS). 2003. Macroeconomic Review 1(2) October 2003. Singapore: Monetary Authority of Singapore.
Sleigh, A. C.; Chee, H. L.; Yeoh, B. S.; Phua, K. H.; and Safman, R. eds. 2006. Population Dynamics and Infectious Diseases in Asia. Singapore: World Scientific.
Takeuchi, Tsutomu 竹内 勤. 2004. Nihon no Kiseichu Shikkan Seiatsu no Keiken o Sekai ni: Hashimoto Initiative 日本の寄生虫疾患制圧の経験を世界に―橋本イニシアティブ[Reporting Japan’s experi ences of parasite infection control to the world]. In Gurobaru Jidai no Kansensho グローバル時代の感染症 [Infectious diseases in the era of globalization], edited by Tsutomu Takeuchi and Hiroki Nakatani 竹内 勤; 中谷比呂樹, pp. 154–185. Tokyo: Keio University Press.
Tambyah, Paul; and Leung, Ping-Chung, eds. 2006. Bird Flu: A Rising Pandemic in Asia and Beyond? Singapore: World Scientific.
Tan, Chorh-Chuan. 2006. SARS in Singapore: Key Lessons from an Epidemic. Annals Academy of Medicine 35(5): 345–349.
Tan, Siok Sun. 2007. Goh Keng Swee: A Portrait. Singapore: Editions Didier Millet.
Tan Tock Seng Hospital (TTSH). 2004. The Silent War: 1 March–31 May 2003. Singapore: Tan Tock Seng Hospital.
Tandon, Ajay. 2005. Population Health and Foreign Direct Investment: Does Poor Health Signal Poor Government Effectiveness? ERD Policy Brieff 33.
Tay, Catherine Swee Kian. 2003. Infectious Diseases Law and SARS. Singapore: Times Media.
Tay, Simon S. C., ed. 2006. A Mandarin and the Making of Public Policy: Reflections by Ngiam Tong Dow. Singapore: NUS Press.
Teo, Peggy; Yeoh, B. S. ; and Ong, S. N. 2005. SARS in Singapore: Surveillance Strategies in a Globalizing City. Health Policy 72: 279–291.
Trocki, Carl A. 2006. Singapore: Wealth, Power and the Culture of Control. New York: Routledge.
Turnbull, C. M. 1982. A History of Singapore 1819–1975. Fourth Impression. London: Oxford University Press.
World Health Organization (WHO). 2007. SARS Control: Control Measures Implemented by the Non-European SARS Affected Countries. Hamburg: WHO. http://survey.erasmusmc.nl/SARSControlproject/picture/upload/Non%20European%20SARSControl%20Measures%20D8%202%20Final.pdf, accessed June 29, 2011.
―. 2006. SARS: How a Global Epidemic Was Stopped. Geneva: WHO Press.
―. 2005. Combating Emerging Infectious Diseases in the South-East Asia Region. New Delhi: WHO.http://www.searo.who.int/LinkFiles/Avian_Flu_combating_emerging_diseases.pdf, accessed August 8, 2011.
―. 2003. Consensus Document on the Epidemiology of Severe Acute Respiratory Syndrome (SARS). Geneva: WHO. (WHO/CDS/CSR/GAR/2003.11) http://www.who.int/csr/sars/en/WHOconsensus.pdf, accessed August 8, 2011.
―. 2000. World Health Report 2000. Geneva: WHO Press.
Yoshikawa, Minako Jen. 2010. Dengue and Chikungunya Virus Infection in Southeast Asia: Active Governmental Intervention in Republic of Singapore. In Current Topics of Infectious Diseases in Japan and Asia, edited by K. Tanaka, Y. Niki, and Y. Akatsuki, pp. 59–77. Tokyo: Springer.
Yoshikawa, M. J.; Tang, C. S.; and Nishibuchi, M. 2010. Incidence of Chikungunya Fever in Singapore: Implications of Public Health Measures and Transnational Movements of People. Tropical Medicine and Health 38(1): 39–45.
* A part of this paper was presented at a roundtable discussion at a conference titled Transnational Policies: Connecting the Asia Pacifi c held in Vancouver, Canada, on March 17–18, 2011. Th is paper forms one chapter of this author’s doctoral thesis that was submitted to the Graduate School of Asian and African Area Studies, Kyoto University, in March 2012. In this paper, the names of ethnic Chinese individuals are presented with family names preceding given names, with the exception of authors’ names. While every eff ort has been made to avoid errors, this author apologizes for any that may have occurred.
1) The figure represents 21 percent of healthcare workers; 95 percent of cases were concentrated in 12 countries/areas of the Western Pacific Region of the WHO (WHO 2006, 185). The “Spanish flu” is believed to have claimed 20 million–100 million lives.
2) An emerging infectious disease refers to a disease “of infectious origin whose incidence in humans has increased within the recent past or threatens to increase in the near future,” including one that has emerged “in new geographic areas or increased abruptly” (WHO 2005, 1).
3) This paper will define a government as a governing body consisting of politicians and public servants engaged in the service of the supreme authority.
4) Morbidity is the condition of illness or abnormality, the rate at which an illness occurs in a particular population or area.
5) A report on the fatality in Virginia and outbreaks in schools across several states in the country was aired on October 16 and 18, 2007, as “the country is on the heels of the national crisis,” by the NBC Nightly News; “silent killer in hospitals, schools and day care centers that are often discovered when it is too late” was aired by the CBS Evening News on October 18, 2007.
6) Although its definition varies, public health is concerned with population health.
7) The ethnic composition of the majority of the population (citizens and permanent residents) was Chinese (74.1 percent), Malays (13.4 percent), Indians (9.2 percent), and others (3.3 percent).
8) Besides port businesses generating movements of goods and people, Changi Airport in Singapore handled in excess of 35 million passengers and 214,000 aircraft in 2006, servicing 183 cities in 57 countries (De Koninck et al. 2008, 60).
9) Interestingly, D. H. Phua et al. (2005) report less psychiatric morbidity among healthcare providers in the emergency department of a hospital in Singapore, pointing out a couple of explanations including unique ties among the staff.
10) An expression used by the Singapore Tourism Board for brand promotion of the city-state.
11) HK Department of Health learned of the index case on February 24, but the linkage to the hotel failed to attract initial attention. The warning pointing to the hotel, arrived from Singapore on March 13 and then the federal health authority Health Canada on March 18. “Only then did the Department of Health start reviewing all its files on reported cases of severe community-acquired pneumonia” (WHO 2006, 142). HK authorities may have an alternative explanation, as detailed in “SARS in Hong Kong: from Experience to Action,” report, http://www.sars-expertcom.gov.hk/english/reports/reports.html, accessed August 9, 2011.
12) The nonspecific initial clinical features include fever (>38°C), chills, headache, malaise, myalgia, and diarrhea. Consequently, 20–25 percent of patients required intensive care (WHO 2006, 178).
13) Local laboratory experts devoted to pursue the new SARS-CoV and development of early diagnostic tests (WHO 2006, 106).
14) Containment is reduction of morbidity and mortality to levels at which the disease is no longer considered to be a public health problem.
15) Now known as the Homefront Crisis Executive Group, the group has been in existence since 1973. The group was activated in the past, for example in 1999 when the Nipah virus infection was imported from Malaysia.
16) On April 23, 250 army personnel were deployed to the MOH for two months (Goh et al. 2006, 302).
17) Established by the PAP, statutory boards are governmental organizations under relevant ministries.
18) Details are at http://www.pa.gov.sg/home.html, accessed August 8, 2011.
19) The PA volunteers included businessmen, members of educational, religious, and other institutions, senior citizens, and members of ladies clubs.
20) HK implemented the policy on March 29, 2003.
21) A MICA officer explained to me in a personal interview in March 2010 that the timing of the channel setup should have been much earlier to be more effective.
22) Since the CDC alone could not respond to the sudden surge in demand to isolate patients, TTSH—located opposite the CDC—used its general wards, which potentially resulted in more cases at the hospital (TTSH 2004, 24).
23) Triage functions were established at polyclinics to screen patients with fever, which reduced the burden on hospitals and facilitated early defection.
24) Rapid identification and isolation as the precautionary measures implemented during the March–May period may have worked to prevent further transmission when a 27-year-old Chinese Singaporean contracted SARS through accidental contamination in a microbiology laboratory in September 2003 (WHO 2006, 46).
25) Personal communication (an e-mail from Dr. Goh Kee Tai, received on October 26, 2007).
26) Personal communication (an e-mail from Dr. Goh Kee Tai, received on October 26, 2007). Goh was the head of the Quarantine and Epidemiology Department, Ministry of the Environment, from 1978 to 2003, and was involved in the revision of the infectious disease legislation in 1976.
27) The Infectious Diseases Act was further amended to ensure compliance with the HQO. According to section 65, offenders could be jailed for up to 6 months and/or fined S$10,000 upon conviction for the first offense, and imprisoned for a term not exceeding 12 months and/or fined S$20,000 for the second and subsequent offenses (Chua 2004, 124–127; Tay 2003, 50). Even the high-profile Madam Kwa Geok Choo, the wife of then Senior Minister Lee Kuan Yew, was quarantined at home after having undergone an ultrasound scan examination at a hospital where a SARS case was reported.
28) The scheme provided self-employed people with S$70 a day and employed people with an amount equal to their daily salary, up to a maximum of S$70 a day, during the quarantine period (Chua 2004, 123).
29) Other sources report slightly different percentages. Certain medical procedures such as aerosolization of respiratory secretions (e.g., intubation: the use of nebulizers, suction, or assisted ventilation) may have caused the transmission in healthcare settings.
30) Personal interview with Tan Wee King in Singapore on August 25, 2007. Her view supports findings by D. H. Phua et al. (2005).
31) Visitor arrivals fell by nearly 100 percent on a seasonally adjusted annualized rate basis (MAS 2003, 10).
32) Dengue virus infection re-emerged in Singapore in the late 1990s, and Singapore scaled up its national control program, especially after the regional outbreak in 2005 (Yoshikawa 2010, 66–67). Singapore controlled the first local outbreak of chikungunya fever quickly and enhanced control measures to deal with the subsequent outbreaks in 2008 (Yoshikawa et al. 2010, 41–42).
33) About a quarter of the territory produced poultry, pork, and half of the vegetables required in 1960 (De Koninck et al. 2008, 40). A midyear estimate of the population in 1965 was 1,864,900 (MOH 1968, 35).
34) Non-seasonally adjusted total unemployment rates for June 1957 and 1970 show 5 percent and 8.2 percent respectively (MTI 2007, 15), and 14 percent is reported right after independence (Lee 2000, 23) and for slightly earlier years (Tan 2007, 85).
35) Devaluation was from USD/GBP 2.80 to 2.40 and caused Singapore to lose 14.3 percent of its sterling reserves, according to Lee (2000, 57). However, Singapore’s civil servant Ngiam Tong Dow said that the devaluation caused only moderate damage (Tay 2006, 45).
36) According to Amitav Acharya, the young country’s strategy to invite MNCs actually ensured committed interests of the developed world in Singapore, which worked to provide the “foundation of its national security” (Acharya 2008, 25, 58).
37) In 1972, 46 percent of new foreign capital invested was from the United States, which became the second largest trade partner by 1973. Other capital providers were Western Europe, Japan, Hong Kong, Taiwan, Malaysia, and Australia (Turnbull 1982, 308). The four top investors in 1980 were: 26.3 percent UK, 22.5 percent US, 11.7 percent Japan, and 1.9 percent the Netherlands (MTI 2007, 12).
38) According to Chong Guan Kwa, Singapore essentially counteracted the weaknesses and disadvantages of a tiny city-state reliant on neighbors for survival (Kwa 2002, 123).
39) N. Ganesan mentions health along with housing and education as areas that were given priority by the PAP in the first two decades (Ganesan 2002, 53).
40) NUS 1967–June 1969, 80 ( ST, August 8, 1968).
41) Rodney King (2008) disagrees with the depiction of the vulnerable and poor conditions of the new nation in 1965, claiming the description as “one of Singapore’s most enduring myths” (ibid. , 7).
42) It is also known that strict quotas of Chinese, Malays, Indians, and others concurrently functioned as a solution to another English legacy: racial division. Although the English language was prioritized at school, given its neutrality and usefulness in business (Lee 2000, 173), the multiracial island-state adopted four official languages—English, Chinese, Malay and Tamil—in the process of fostering national cohesion. Since several dialects of Chinese were used, a common use of Mandarin Chinese was promoted in the “Speak Mandarin” campaign that started in 1978. Although the evaluation of Singapore’s education and language policy is beyond the scope of this paper, the government’s attention proved to be beneficial owing to the important role of languages in disseminating information relating to health.
43) It is probable that altruism was not the only factor. Defense, too, was a consideration since the PAP government had implemented a conscription system, now known as the National Service, starting from 1970 in response to the British withdrawal (Lee 2000, 42).
44) NUS June 1969–1970, 153 ( ST, August 5, 1970).
45) Although Edwin Lee (2008) notes that Singapore inherited civil services “in good working order” from the suzerain ( ibid. , 266), the health services left behind by the British were vulnerable (Barr 2005, 147).
46) Speech by Lee Kuan Yew at the fourth National Medial Convention dinner of the Singapore Medical Association (NUS January–June 1972, 69–70 ( ST, March 26, 1972)).
47) Licensing of all hawkers was implemented in 1966 (Singapore Government 1967, 310).
48) The ministry was established after Lee Kuan Yew set “an official national goal” to clean Singapore’s waterways (Dobbs 2003, 103), especially the Singapore River.
49) Minister of Health, Yong Nyuk Lin proclaimed the start of a campaign to inform people of their responsibility to keep the nation clean. The previous law was amended to apply “more punitive penalties for those littering public streets, drains and vacant sites on the island” (NUS 1967–June 1969, 18 ( ST, May 25, 1967)). The anti-spitting campaigns in the 1960s cautioned the act would spread diseases like tuberculosis (Lee 2000, 199). A two-week “Great Singapore Smokeout” campaign was carried out in December 1980 (NUS 1979–1980, 328 ( ST, December 16, 1980)).
50) These include oil-refining, petrochemicals, banking, tourism, semiconductors, telecommunications, electronics, and biomedicine. Today, the nation commands economic power that is disproportionate to the size of its territory and its total population of about five million.
51) Similarly, referring to colonial days, Phua notes that a study could have been attempted on the relationship between health and development or human capital investment for the mining and plantation industries if reliable details had been available (Phua 1989, 322).
52) Goh was minister for health (1981–82), second minister of health (1982–84), first deputy prime minister (1985–90), and prime minister (1990–2004).
53) Bengal cholera is caused by a new cholera biotype, Vibrio cholerae O139.
54) Lee Kuan Yew and Goh Chok Tong resigned from the cabinet as the minister mentor and the senior minister, respectively, after the election.
55) Singapore’s Gini coefficient score—measuring income gap—stood at one of the world’s highest, 0.425 in 2008 (Han et al. 2011, 143).
56) In addition, anti-dengue events hosted by Singapore jointly with the WHO annually since 2008 are encouraging, as Singapore’s comprehensive vector control has so far resulted in moderate prevalence of domestic transmission (Yoshikawa 2010, 59).